Endometrial cancer
Key facts
- Endometrial cancer starts when the lining of the uterus (endometrium) grows abnormally and in an uncontrolled way.
- The most common symptom is unusual vaginal bleeding.
- Other signs can include watery discharge, unexplained weight loss, pain in the abdomen (tummy), or trouble urinating.
- Treatment may include surgery, radiotherapy, chemotherapy or hormone therapy.
- If you notice any unexpected vaginal bleeding, see your doctor to find out the cause.
What is endometrial cancer?
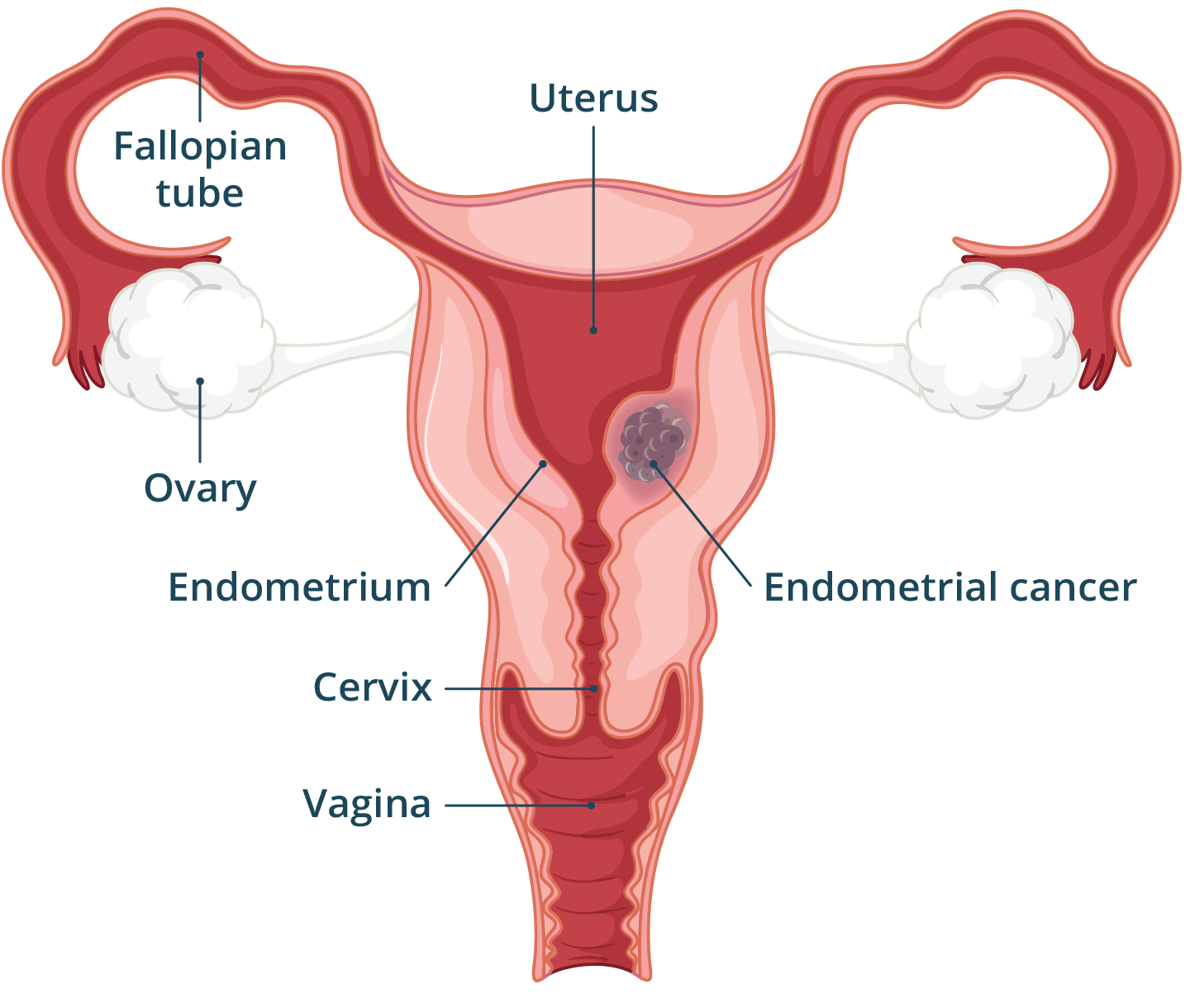
Endometrial cancer develops when the cells lining the uterus — known as the endometrium — grow in an abnormal and uncontrolled way. It is the most common cancer of the female reproductive system.
Endometrial cancer is more common in females over 50 years of age who have gone through menopause. Younger females, transgender males and intersex people can also develop endometrial cancer.
Endometrial cancer is grouped into 4 main stages:
- Stage I: Cancer is only in the uterus.
- Stage II: Cancer has spread from the uterus to the cervix.
- Stage III: Cancer has spread beyond the uterus and cervix but remains within the pelvis. It may involve the ovaries, fallopian tubes, vagina or lymph nodes of the pelvis or abdomen.
- Stage IV: Cancer has spread to other parts of the body such as the bladder, bowel, abdomen or organs such as the lungs or brain.
Most people with endometrial cancer recover, because it is often found early.
What are the symptoms of endometrial cancer?
One of the first signs of endometrial cancer can be unusual vaginal bleeding, especially bleeding after menopause.
Other signs and symptoms can include:
- bleeding between periods
- changes in your periods, such as heavier periods or constant bleeding
- watery, blood-tinged or otherwise unusual vaginal discharge
- unexplained weight loss
- trouble urinating (weeing)
- pain in the pelvic area
- pain during sex
These symptoms can happen for many other reasons, and don't always mean you have cancer. It's important to see a doctor to find out what's causing them.
CHECK YOUR SYMPTOMS — Use the Symptom Checker and find out if you need to seek medical help.
What causes endometrial cancer?
The exact cause of endometrial cancer isn't clear, but some risk factors are known. Some risks can be lowered by making changes to your lifestyle.
Risk factors related to your general health include:
- living with obesity or diabetes
- smoking
- older age and have gone through menopause
- taking tamoxifen (a medicine that treats breast cancer)
- having Lynch syndrome (also called hereditary non-polyposis colorectal cancer — HNPCC)
Risk factors linked to your reproductive health include if you:
- have endometrial hyperplasia (thickening of the lining of the uterus)
- started periods before the age of 12 years or menopause after 55 years of age
- use oestrogen-only hormone therapy for menopause
- have never been pregnant
- have a tumour in one of your ovaries
- have polycystic ovary syndrome (PCOS)
When should I see my doctor?
If you notice any of the symptoms of endometrial cancer, including unexpected vaginal bleeding, see your doctor. These symptoms are common and don't always mean cancer, but it's still important to get checked. You can ask to see a female doctor if you prefer.
ASK YOUR DOCTOR — Preparing for an appointment? Use the Question Builder for general tips on what to ask your GP or specialist.
How is endometrial cancer diagnosed?
If you have symptoms that might mean endometrial cancer, your doctor will ask about your health, symptoms and family history of cancer.
Your doctor will do a physical and pelvic examination, which may include cervical screening.
This includes using a medical tool called a speculum to look inside your vagina. They may also feel your uterus by placing 2 fingers inside your vagina and their other hand on your abdomen. You can ask for a nurse or support person to be present during this examination.
You may also have blood test s and a transvaginal pelvic ultrasound (TVS). If you prefer, you can ask to see a female health professional.
Your doctor may refer you to a gynaecologist for more tests if they want to check for endometrial cancer. If a cancer is found, they will refer you or consult with a gynaecological oncologist — a doctor who specialises in cancers of the female reproductive system.
An endometrial biopsy is the main test used to confirm endometrial cancer. It involves taking a small sample of tissue from the lining of your uterus (endometrium) to look for cancer or abnormal cells under a microscope.
This is usually done in a gynaecology clinic using a thin, flexible tube (called a pipelle). If a clear diagnosis is not found you may need another biopsy done during a hysterectomy, or a dilatation and curettage ('D&C'). This is usually done in a day surgery clinic under anaesthetic.
You can take pain relief before the biopsy — ask your doctor which option is best for you. It's common to have mild cramping or light bleeding for up to a week after the test.
In some cases, you may also need imaging tests such as a computed tomography (CT), magnetic resonance imaging (MRI) or positron emission tomography (PET) scan to check if the cancer has spread.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How is endometrial cancer treated?
Treatment for endometrial cancer depends on the stage of the disease, your general health and your preferences, such as if you wish to have children in the future. For most people, surgery is the main treatment.
Other treatments may also be recommended, depending on the cancer and if it has spread. These include:
- radiotherapy (also called radiation therapy)
- chemotherapy
- hormone therapy
- emerging therapies, such as targeted therapies and immunotherapy
Surgery
Surgery is the main treatment for most cases of endometrial cancer. The type of surgery depends on many factors such as your age, other medical conditions, overall health and your fertility preferences.
For early stage cancer in the uterus only, standard surgery usually includes:
- total hysterectomy — removal of the uterus and cervix
- bilateral salpingo-oophorectomy — removal of both fallopian tubes and ovaries
- pelvic lymph node assessment or sentinel lymph node biopsy
Depending on your cancer, your doctor may recommend removing your pelvic lymph nodes. This is known as a lymphadenectomy.
Radiotherapy
Radiotherapy (radiation therapy) uses x-ray beams to kill or damage cancer cells.
Radiotherapy is often used after surgery to lower the chance of the cancer coming back. It works by stopping cancer cells from growing or spreading, while limiting damage to healthy tissues.
Radiotherapy may be external (when you lie near a machine that aims x-rays at your cancer), or internal (also known as brachytherapy, where a small radioactive device is placed inside your body for a few minutes).
Hormone therapy
Hormone therapy can help treat some types of endometrial cancer, especially when the cancer cells respond to the hormones oestrogen and progesterone. It's often used for people with low-grade disease, advanced cancer, or if surgery can't be done or you want to have children in the future.
Hormone therapy can be taken as tablets, or by using a hormone-releasing intrauterine device (IUD) which your doctor places in your uterus.
Chemotherapy
Chemotherapy uses medicines to kill or slow the growth of cancer cells, while aiming to cause as little harm as possible to healthy cells. Chemotherapy is usually given directly into the vein (called IV). Most people need several treatment sessions, called cycles, over weeks or months.
Chemotherapy may be given in a day clinic in hospital, depending on your situation.
Emerging therapies
New treatments for endometrial cancer are being developed using genetic and other advanced tests. These include targeted therapy, immunotherapy and combination treatments.
Immunotherapy is a type of cancer treatment that helps your immune system find and attack cancer cells more effectively. It works by boosting your body's natural defences so they can destroy cancer cells while leaving most healthy cells unharmed.
Read more on cancer immunotherapy.
Targeted therapy uses medicines that attack specific parts of cancer cells to help stop the cancer growing or spreading. These medicines travel through the body similar to chemotherapy, but work in a more focused way and often cause fewer side effects.
Read more on targeted therapy.
Living with endometrial cancer
If you need to talk to someone about your mental health, call Beyond Blue on 1300 22 4636.
Treatment for endometrial cancer can lead to changes in your bladder, bowel and sexual function.
It is common to have a wide range of emotions — you may feel worried, sad or scared that the cancer might come back.
Talk to a counsellor, social worker or support group to help you manage these feelings.
Keeping a healthy lifestyle including eating well, being active and getting enough sleep can help your recovery and general health.
It is important to go to all your follow-up appointments and tell your doctor about any new symptoms. Regular check-ups can help find any return of cancer early so treatment can start straight away.
Remember, living with cancer isn't just about managing the disease. Take care of yourself, get support and try to keep doing the things you enjoy.
What are the complications of endometrial cancer?
Endometrial cancer and its treatment can cause a range of physical and emotional challenges. These can include the effects of surgery, chemotherapy, radiotherapy and hormone therapy. Each can have different complications.
Endometrial cancer is often found early and most people recover. But if it isn't found early, the cancer can spread and grow into the muscle of the uterus, nearby lymph nodes, or other parts of the body such as the lungs, liver, bones or brain.
Menopause
If you haven't been through menopause, some treatments for endometrial cancer can bring it on suddenly. Talk to your healthcare team about how to manage symptoms of menopause.
Infertility
Some treatments for endometrial cancer can affect your ability to get pregnant. Surgery to remove your uterus or radiation to your pelvis can make pregnancy impossible. In some early cases, treatment that preserves fertility may be possible. Talk with your healthcare team about your options and what might be right for you.
Other complications
Other complications you may experience after treatment for endometrial cancer include:
- fatigue
- changes in your bowel and bladder
- lymphoedema
- anaemia
- changes to your sexuality — how you feel about sex, how you respond sexually, or physical changes such as vaginal dryness
Your medical team, social workers or support organisations can help you manage these changes.
Can endometrial cancer be prevented?
There is no sure way to prevent endometrial cancer, but you can lower your risk by:
- maintaining a healthy weight
- taking combined oral contraceptives ('the pill')
- including progesterone therapy as part of menopausal hormone therapy (also known as MHT or HRT), if you still have your uterus
If you have a high risk of endometrial cancer, you may choose to have surgery to remove your uterus (known as a risk-reducing hysterectomy). Your doctor may recommend this if you have a condition called atypical endometrial hyperplasia or a genetic condition such as Lynch syndrome. If you're thinking about this, talk to a specialist, such as a doctor at a familial cancer clinic, about the risks and benefits.
Resources and support
The Cancer Council has information for people living with cancer and their families:
- Uterine cancer booklet.
- Support and services for Australians affected by cancer.
- Practical and financial help, including support with transport, accommodation, costs and legal issues.
- Resources on living with cancer that include emotional and practical information.
You can check your cancer risk with Cancer Australia's calculator.
Languages other than English
- The Cancer Council has information for people with cancer and their families in community languages.
- General information about cancer is available from NSW Health in many community languages.
Information for Aboriginal and/or Torres Strait Islander peoples
- Cancer Council NSW has information about cancer for Aboriginal and/or Torres Strait Islander peoples.
- Our Mob and Cancer is an Australian Government website with information and resources for Aboriginal and/or Torres Strait Islander peoples.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: October 2025


















