Psoriasis
Key facts
- Psoriasis is a long-term skin condition that causes red, scaly patches on your skin.
- It can also affect your nails and joints.
- Psoriasis is not contagious (it can't be caught from others).
- Flare-ups may be triggered by stress, cold weather or infections.
- There is no cure, but treatment can help manage your symptoms.
What is psoriasis?
Psoriasis is a long-term (chronic) condition that may cause red, itchy, scaly patches on your skin. It happens when your immune system makes skin cells grow too fast. Psoriasis tends to come and go over time.
There are different types of psoriasis, and each can look different. It may appear on many parts of the body, including your:
- scalp (the skin on your head)
- hands
- feet
- elbows
- back
- fingernails or toenails
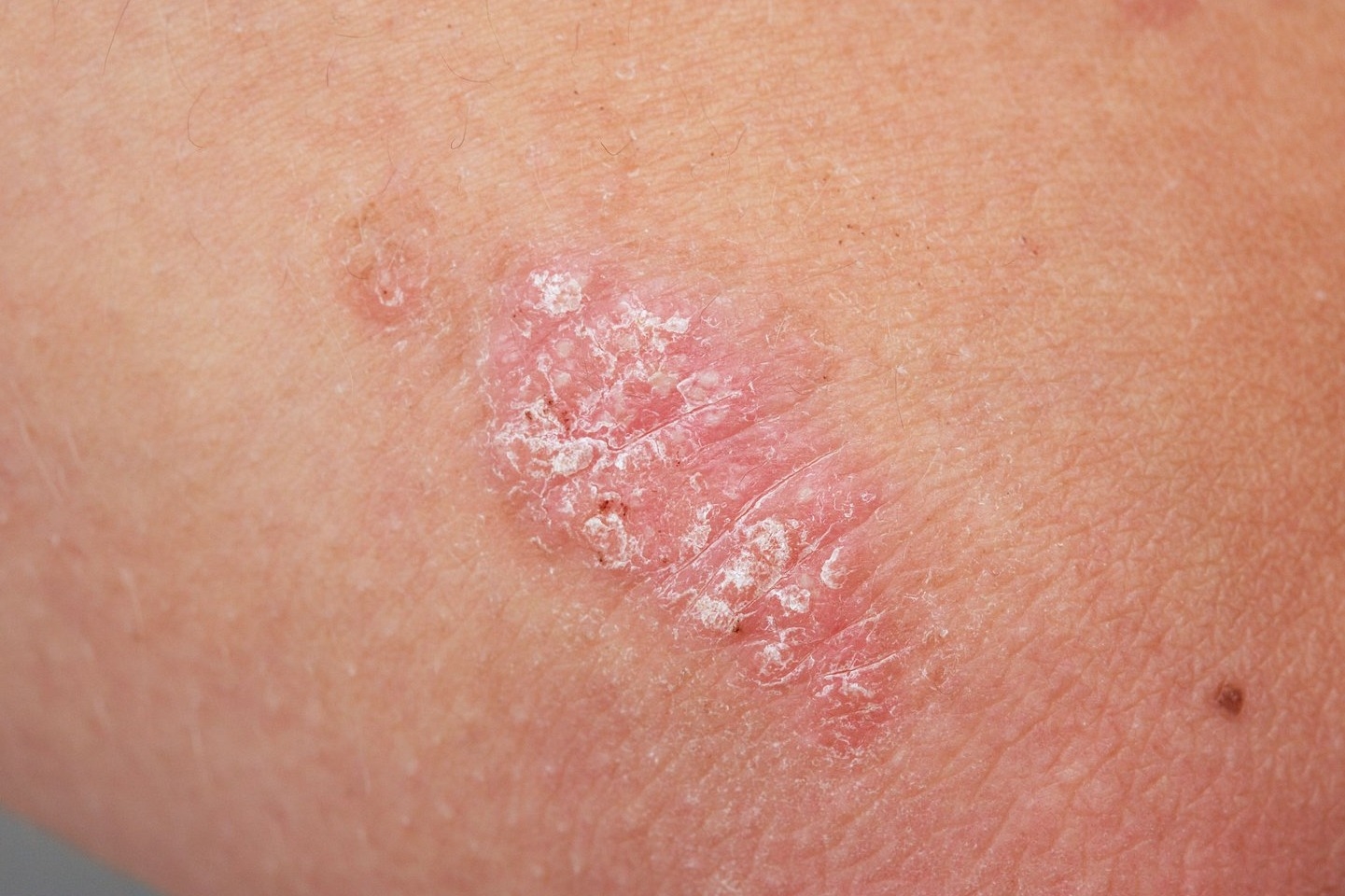
Psoriasis is not contagious. This means you can't catch it from someone else.
What are the symptoms of psoriasis?
There are several types of psoriasis. Each type may look and feel different and can affect different parts of your body.
Plaque psoriasis
Plaque psoriasis is the most common type of psoriasis. The symptoms:
- include raised, red patches of skin covered with silvery scales
- often affect the elbows, knees, lower back and scalp
- may cause your skin to feel dry, itchy and sore
Nail psoriasis
Nail psoriasis affects the fingernails and toenails. It may lead to:
- pitting, thickening or discolouration of your nails
- nails lifting from the nail bed
- crumbly or damaged nails
Inverse psoriasis
Inverse psoriasis affects skin folds, such as:
- under your breasts
- in your groin
- around your buttocks
It may look like smooth, red patches of skin that get worse with sweating or rubbing. It may be triggered by fungal infections.
Guttate psoriasis
Guttate psoriasis often starts in children or young adults. It may be triggered by infections, especially strep throat.
Symptoms may show as small, drop-shaped spots on your torso, arms and legs.
Pustular psoriasis
If you have symptoms of pustular psoriasis, see your doctor or go to the nearest hospital emergency department.
Pustular psoriasis may lead to yellow or white blisters filled with non-infectious pus (pustules). It may affect your hands and feet.
This type may sometimes lead to fever and swelling in your arms and legs. These are serious complications and you may need emergency care in hospital to treat this condition.
Erythrodermic psoriasis
Erythrodermic psoriasisleads to widespread redness and peeling of the skin. Your skin may feel hot, itchy and painful.
Psoriatic arthritis
Psoriatic arthritis affects the joints and areas where tendons attach to bones. It may lead to:
- joint pain
- joint swelling
- joint stiffness
It often happens in people who already have skin psoriasis.
CHECK YOUR SYMPTOMS — Use the Symptom Checker and find out if you need to seek medical help.
What causes psoriasis?
Psoriasis is an immune system condition. It's not clear exactly what causes it but your genes may play a part. This means if someone in your family has psoriasis, you may be more likely to get it too.
A range of things can trigger or make psoriasis worse, including:
- infections
- stress
- cold weather
- skin injuries
- smoking
- some medicines
When should I see my doctor?
See your doctor if you notice red, scaly or raised patches on your skin that don't go away.
If you are diagnosed with psoriasis, see your doctor if:
- it becomes worse or spreads
- you feel discomfort or pain
- you're worried about your symptoms
- it doesn't get better with treatment
- you have painful, swollen or stiff joints
When to seek urgent care
Some types of psoriasis, such as pustular psoriasis, may be serious and may need urgent care.
If you feel unwell, or you suddenly develop a full-body red rash, see a doctor straight away.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How is psoriasis diagnosed?
Your doctor may diagnose psoriasis by looking at your skin. They may also ask you about your family's medical history.
Your doctor may refer you to a dermatologist for further tests, or to a rheumatologist if your joints are affected.
Sometimes, a small skin sample (called a biopsy) may be taken to confirm the diagnosis.
ASK YOUR DOCTOR — Preparing for an appointment? Use the Question Builder for general tips on what to ask your GP or specialist.
How is psoriasis treated?
There is no cure for psoriasis but there are many treatments that may help manage it. What works best depends on how severe your psoriasis is and where it appears on your body.
Treatments may include:
- topical creams and ointments — these may include steroid creams or vitamin D creams
- light therapy — which uses special ultraviolet (UV) light, called phototherapy
- medicines — tablets or injections that help control your immune system
- biological medicines — these are tailored to each person, so talk with your dermatologist or rheumatologist about your options
LOOKING FOR A MEDICINE? — To search by brand name or active ingredient, use the Medicines information search feature.
Living with psoriasis
Living with psoriasis can be challenging, but there are ways to manage your symptoms. Here are some tips that may help:
- Moisturise your skin daily — this may help reduce dryness and itching. Ask your doctor to recommend a moisturiser that's right for you.
- Follow your treatment plan — take your medicines as directed by your doctor to help keep psoriasis under control.
- Reduce stress — stress can make psoriasis worse. Try relaxation techniques, such as deep breathing, gentle exercise or speaking to a counsellor.
- Live a healthy lifestyle — eating well and staying active may reduce flare-ups.
- Quit smoking — smoking can trigger psoriasis and make it worse. Ask your doctor for support if you want to quit.
What are the complications of psoriasis?
Psoriasis may affect your whole body and wellbeing. Some people may develop:
- psoriatic arthritis, which may damage the affected joints
- low mood or emotional stress, including depression
- increased chance of other health problems, such as inflammatory bowel disease, diabetes, heart disease or liver disease
Psoriasis can also affect your social life. The skin rash might make you feel self-conscious, and harder to go out or spend time with others.
Can psoriasis be prevented?
There is no known way to prevent psoriasis. You can help reduce flare-ups by following your treatment plan.
Resources and support
For more information about psoriasis, see the following websites:
You can also call the healthdirect helpline on 1800 022 222 (known as NURSE-ON-CALL in Victoria). A registered nurse is available 24 hours a day, 7 days a week.
Languages other than English
Health Translations offers translated information on several topics, such as:
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: April 2025














