Cholesterol
Key facts
- Cholesterol is a type of fat produced by your body and is also found in some foods.
- Cholesterol is important for your body to build and repair cells and to make hormones.
- Two main types of cholesterol are LDL known as 'bad' cholesterol and HDL known as 'good' cholesterol.
- Too much 'bad' cholesterol can damage your arteries and increase your risk of heart disease and stroke.
- Lifestyle changes and medicines can help lower high cholesterol.
What is cholesterol?
Cholesterol is a type of fat produced by your body and can also be found in food. Most of the cholesterol in your body is produced by your liver; the rest comes from the food you eat.
Your body needs cholesterol to build and repair cells, and to make hormones. While it is needed for good health, too much 'bad' cholesterol can cause fatty deposits called plaque to form in the walls of your arteries. This leads to a narrowing and hardening of the arteries, which damage your arteries and increase your risk of heart disease and stroke.
High cholesterol is common among Australians, with more than 2 in 5 adults living with high cholesterol.
What are the types of cholesterol?
There are different types of cholesterol. Each is named after the different proteins that carry cholesterol (lipoproteins) in the blood. The main types of lipoproteins are high-density lipoprotein (HDL) and low-density lipoprotein (LDL).
- HDL cholesterol is known as 'good' cholesterol. This is because HDL helps remove cholesterol from your arteries by carrying cholesterol back to your liver for disposal.
- LDL cholesterol is known as 'bad' cholesterol. This is because LDL leaves cholesterol in your arteries.
Triglycerides are a type of fat in your blood that can also increase your risk of heart disease. Triglycerides are usually tested along with cholesterol when you have a cholesterol blood test.
Some foods also contain cholesterol. Foods that contain dietary cholesterol include:
- liver
- egg yolks
- pate
- kidneys
- prawns
What are signs and symptoms of high cholesterol?
Many people don't know they have high cholesterol because there are no obvious symptoms.
If left untreated, high cholesterol can increase the risk of serious health conditions. It is important to check if you have high cholesterol with regular check-ups and blood tests.
Some people have a condition called familial hypercholesterolaemia. This is where a genetic problem leads to high cholesterol. About 1 in 250 people have this condition, and many don't know they have it.
What causes high cholesterol?
There is no single cause of high cholesterol, but factors that increase your risk include:
- older age
- smoking
- increased alcohol use
- lack of physical activity
- family history
- unhealthy diet
- overweight or obesity
What are the risks linked to high cholesterol?
Although some cholesterol is needed for your body to function, too much LDL (bad) cholesterol in the blood can increase your risk of heart and cardiovascular disease, such as heart attack and stroke.
Too much LDL cholesterol leads to fatty deposits called plaque forming in the artery walls. Over time, the plaque causes narrowing and hardening of the arteries (known as atherosclerosis).
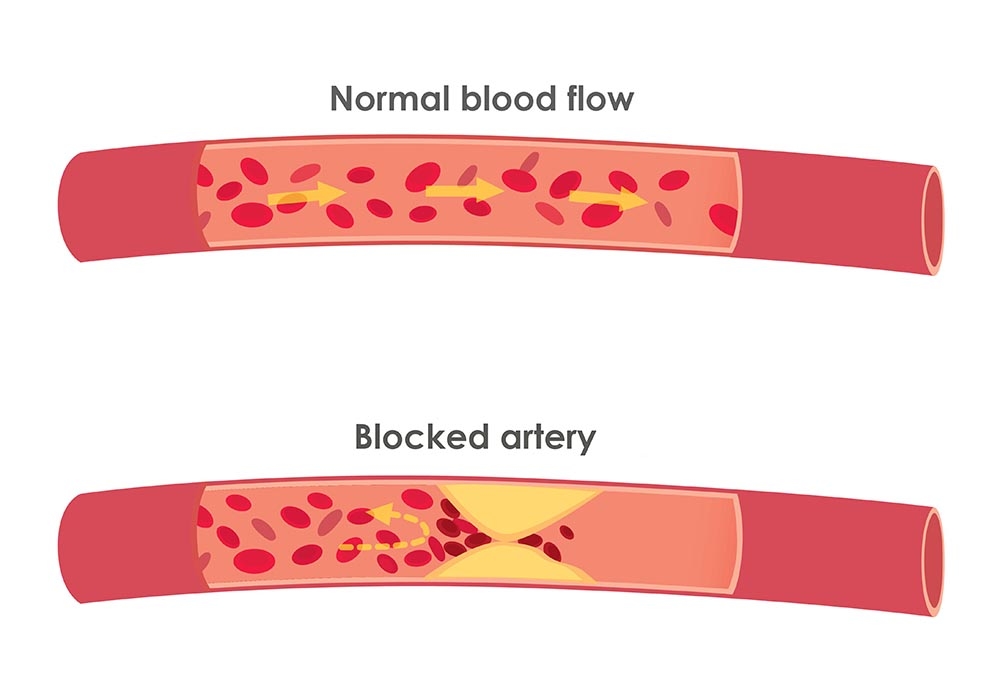
Excess cholesterol in the blood can stick to the walls of your arteries. This is called plaque and can narrow or block arteries completely.
This can lead to:
- Angina — When plaque builds up in the major arteries that supply your heart (coronary arteries) they become narrower and can become partially blocked, reducing blood flow and oxygen supply to the heart. This may cause shortness of breath and chest pain.
- Heart attack — If plaque in a coronary artery bursts (ruptures), a clot may form and block the supply of blood to the heart, starving it of oxygen.
- Stroke — If the blood vessels that supply the brain become narrower or blocked by plaque, blood supply to the brain can be severely reduced or cut off, causing a stroke. Strokes can also be caused when a clot from another part of the body travels through the blood and lodges in an artery in the brain.
- Peripheral vascular disease — This usually affects the arteries that supply the legs and feet, causing leg pain when walking (known as intermittent claudication), and even pain when resting, when the circulation is more badly affected.
When should I see my doctor?
Ask your doctor about having a cholesterol check if you:
- have a family history of high cholesterol or of heart disease
- are 45 years or older
- are 30 years or older and you identify as Aboriginal and/or Torres Strait Islander
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How is high cholesterol diagnosed?
Cholesterol is checked using a blood test called a 'lipid profile 'or 'lipid panel'. This measures total cholesterol, HDL cholesterol and LDL cholesterol, as well as triglycerides.
Your health team may ask you to fast (not eat anything) and only drink water for 8 to 12 hours before the test. You can check with your doctor.
How often should I have my cholesterol tested?
If you are 45 years old, you should have your blood lipids measured every 5 years. Aboriginal and/or Torres Strait Islander people should start having their blood lipids checked at 35 years of age.
All Australians in these age groups are eligible for a regular 20-minute heart health check with their doctor. This includes checks of your blood pressure, cholesterol and blood sugar levels. Your doctor can use your results to assess your risk of having a heart attack or stroke in the next 5 years.
What lifestyle changes can I make to lower my cholesterol?
Here are some tips to lower your cholesterol through lifestyle changes. Some people will only need to improve their lifestyle and diet to get their cholesterol to a safe level. Others may need to take cholesterol-lowering medicines as well.
Reduce your intake of saturated and trans fats
Some fats are important for a healthy diet. You can adopt and follow a healthy diet that's low in saturated and trans fats. A diet high in these fats can raise levels of LDL cholesterol in the blood.
Saturated fat is found in:
- cakes and biscuits
- fatty cuts of meat
- butter and full-fat dairy products
- foods containing coconut or palm oil
Trans fats are found in:
- store-bought baked goods
- snack foods
- deep-fried foods
There is strong evidence that trans fats increase levels of LDL cholesterol in the blood, while decreasing levels of HDL (good) cholesterol.
Replace saturated fats with healthier fats
Replacing foods that contain mainly saturated fats with foods that contain unsaturated fats — such as polyunsaturated and monounsaturated fats — will help reduce your cholesterol level.
For example, instead of butter and cream in cooking, use olive oil, nut butters or avocado.
Healthy unsaturated fats are found in:
- nuts (such as almonds and walnuts)
- olives
- oily fish (for example, salmon and tuna)
- avocado
- seeds (flaxseeds, sunflower seeds, pumpkin seeds)
- oils made from plants and seeds (olive oil, peanut oil, canola oil, soybean oil)
Eat more soluble fibre and plant sterols
Soluble fibre can reduce the absorption of cholesterol into your blood. It slows down digestion and makes you feel fuller for longer. Foods that are high in soluble fibre include:
- oats
- lentils, peas and beans
- psyllium
- barley
- fruits and vegetables (such as apples and carrots)
Plant sterols can lower LDL cholesterol and are found in a range of plant foods such as:
- fruits
- vegetables
- legumes
- nuts and grains
Some are added to some packaged foods, such as table spreads, cereals, low-fat yoghurt and low-fat milk.
Eating 2 to 3 grams of plant sterol-enriched foods daily has been shown to lower LDL cholesterol. If you are pregnant or breastfeeding, speak with your doctor before using plant sterol-enriched products.
Increase your physical activity
Physical activity can help increase levels of HDL cholesterol. Aerobic or cardio exercises and resistance training are particularly effective at controlling your cholesterol levels.
If you haven't been exercising much lately, gradually build up to the recommended amount of physical activity:
- People aged 18 – 64 years should aim for 30 to 60 minutes of moderate-intensity physical activity on most days of the week.
- People aged 65 years and over should aim for a total of 30 minutes of moderate physical activity on most days. You can break this up into smaller periods over the course of the day — for example 10 minutes, 3 times a day.
Maintain a healthy weight
If you are living with overweight or obesity, losing weight can help reduce your levels of LDL cholesterol and triglycerides while increasing your levels of HDL cholesterol.
Other tips to improve your cholesterol levels include:
- limit your alcohol intake
- quit smoking
How can I lower my cholesterol with medicines?
The medicines most often used to lower cholesterol are called statins.
Your doctor may recommend medicine to help lower your cholesterol and reduce your risk of heart attack or stroke.
If you've already had a heart attack or stroke, taking statins can significantly lower your risk of having another one.
Statins work by slowing the amount of cholesterol made in your liver. In response, your liver uses the cholesterol already in your blood to make up for the deficit. This lowers the level of LDL cholesterol in your blood.
If statins alone do not lower your cholesterol enough, you may need additional medicines.
Speak with your doctor if your medicines are causing any side effects, as there may be things you can do to help.
Resources and support
If you have any further questions regarding your cholesterol, you can call the healthdirect helpline on 1800 022 222 (known as NURSE-ON-CALL in Victoria). A registered nurse is available 24 hours a day, 7 days a week.
You can also find further information from organisations such as:
- The Heart Foundation — information about what high cholesterol is and how it can increase your risk of heart disease.
- Familial Hypercholesterolemia Australia Network — information about familial hypercholesterolaemia.
- Eatforhealth by the Australian Government — detailed information and a summary book about the Australian dietary guidelines.
- Dietitians Australia — further information about fats and diet and nutrition health advice.
An accredited practising dietitian can design a personalised eating plan for you to lower your cholesterol. You can find one at Dietitians Australia.
If you smoke, your doctor can help you quit. You can also call the Quitline on 13 7848 to talk to a counsellor, or use its online chat service.
Looking for information for Aboriginal and/or Torres Strait Islander people?
- St Vincent's Hospital Heart Health has an informative video on ways to improve your cholesterol.
- Aboriginal Quitline support Aboriginal and Torres Strait Islander people who smoke to quit smoking.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: May 2024







-cb4909.png)








