Surgery for diverticular disease
What is diverticular disease?
Diverticular disease is the name given to a condition where pouches form in the lining of your colon (large bowel). Most people with diverticular disease have few, if any, symptoms. However, a small proportion do have enough problems to need surgery to remove the affected portion of their bowel.
Diverticular disease is probably caused by too little fibre in the diet over many years. This results in high pressure within your bowel as your bowel tries to squeeze a relatively low volume of solid matter towards your back passage. The pressure causes the wall of your bowel to weaken at certain points, causing pouches to form in the lining of your bowel that bulge through the muscle wall.
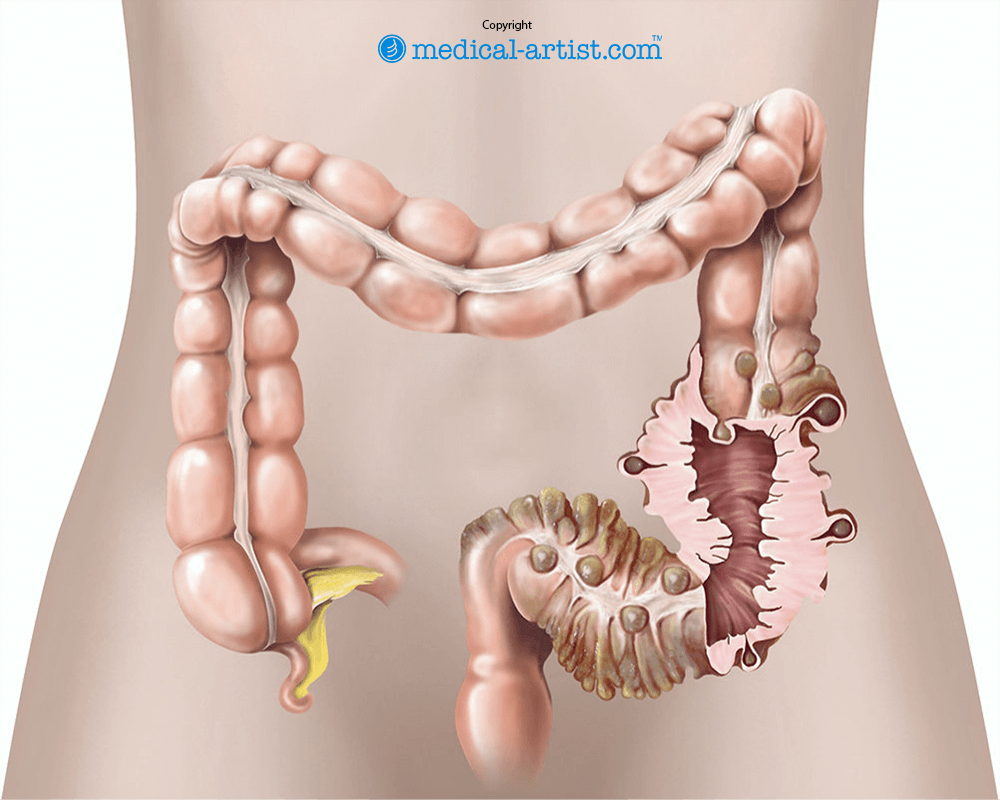
The disease can also cause one or more of the following problems:
- A painful lump in your abdomen caused by inflammation.
- The scars that form when the inflammation has healed cause a narrowing (stricture) in your bowel.
- An abscess can form and make a hole through the wall of your bowel.
- Inflamed diverticulae can stick to other organs in your abdomen (usually your bladder), causing an abnormal connection (fistula) to develop between them.
- Sometimes the inflamed diverticulae will wear down a nearby blood vessel, causing heavy bleeding through your back passage.
What are the benefits of surgery?
You should no longer have the symptoms that are caused by diverticular disease and your quality of life should improve.
Are there any alternatives to surgery?
Painful episodes of diverticular disease may be treated with repeated courses of antibiotics. Increasing the amount of fibre in your diet may help but the diverticulae will not get better.
If a fistula has developed, it will probably not heal without surgery.
What will happen if I decide not to have the operation?
The symptoms that you are experiencing will probably continue and may get worse.
What does the operation involve?
The operation is performed under a general anaesthetic and usually takes 2 to 3 hours.
Your surgeon will remove part of your colon.
Your surgeon will usually join the ends of your bowel back together inside your abdomen.
For safety reasons, they may make a stoma (your bowel opening onto your skin).
How can I prepare myself for the operation?
If you smoke, stopping smoking now may reduce your risk of developing complications and will improve your long-term health.
Try to maintain a healthy weight. You have a higher risk of developing complications if you are overweight.
Regular exercise should help to prepare you for the operation, help you to recover and improve your long-term health. Before you start exercising, ask the healthcare team or your GP for advice.
Speak to the healthcare team about any vaccinations you might need to reduce your risk of serious illness while you recover. When you come into hospital, practise hand washing and wear a face covering when asked.
What complications can happen?
The healthcare team will try to reduce the risk of complications.
Any numbers which relate to risk are from studies of people who have had this operation. Your doctor may be able to tell you if the risk of a complication is higher or lower for you. Some risks are higher if you are older, obese, you are a smoker or have other health problems. These health problems include diabetes, heart disease or lung disease.
Some complications can be serious.
General complications of any operation
- Bleeding during or after the operation. You may need a blood transfusion or another operation.
- Developing a hernia in the scar.
- Infection of the surgical site (wound).
- Allergic reaction to the equipment, materials or medication.
- Acute kidney injury.
- Blood clot in your leg (deep-vein thrombosis – DVT).
- Blood clot in your lung (pulmonary embolus), if a blood clot moves through your bloodstream to your lungs.
- Chest infection. Your risk will be lower if you have stopped smoking and you are free of COVID-19. (coronavirus) symptoms for at least 7 weeks before the operation.
- Difficulty passing urine.
Specific complications of this operation
Keyhole surgery complications
- Damage to structures such as your bowel, bladder or blood vessels when inserting instruments into your abdomen. If an injury does happen, you may need open surgery.
- Developing a hernia near one of the cuts used to insert the ports.
- Surgical emphysema (a crackling sensation in your skin caused by trapped carbon dioxide).
- Gas embolism. This is when gas (carbon dioxide) gets into the bloodstream and blocks a blood vessel.
Complications of surgery for diverticular disease
- Anastomotic leak. This is a serious complication. You will often need another operation.
- Continued bowel paralysis (ileus), where your bowel stops working for more than a few days, causing you to become bloated and to be sick.
- Damage to other structures inside your abdomen.
- Tissues can join together in an abnormal way.
- Compartment syndrome causing pain and damage to your legs.
- The problem coming back. You may need another procedure to fix it.
- Death. The risk is less the fitter you are.
Consequences of this procedure
- pain
- unsightly scarring of your skin
How soon will I recover?
It is usual for your bowel to stop working for a few days.
If you have a temporary or permanent stoma, you will need to learn how to change the bag and care for your stoma.
You should be able to go home after 2 to 10 days.
It may take up to 3 months for you to recover fully.
It is not unusual for your bowels to be more loose than they were before the operation and for you to need to go to the toilet more often each day. This is normal and should improve with time.
If you have a stoma, it will take time for you to become confident with it.
Regular exercise should help you to return to normal activities as soon as possible. Before you start exercising, ask the healthcare team or your GP for advice.
Most people make a good recovery. However, diverticular disease can come back.
Summary
Diverticular disease of the colon can cause pain and other serious problems. Surgery to remove the affected part of your bowel should prevent your symptoms from coming back.
IMPORTANT INFORMATION
The operation and treatment information on this page is published under license by Healthdirect Australia from EIDO Healthcare Australia and is protected by copyright laws. Other than for your personal, non-commercial use, you may not copy, print out, download or otherwise reproduce any of the information. The information should not replace advice that your relevant health professional would give you. Medical Illustration Copyright © Medical-Artist.com.
For more on how this information was prepared, click here.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: January 2026



rendition-574c0b.png)










