Endometriosis
Key facts
- Endometriosis is when tissue that is similar to the inner lining of the uterus grows in other parts of the body.
- Endometriosis symptoms can vary and may include inflammation and pain.
- Some people with endometriosis find it hard to become pregnant.
- There are 4 stages of endometriosis, but having a higher stage does not mean you have more pain.
- Treatment can include medicine, surgery or other types of support.
What is endometriosis?
Endometriosis is when body tissue similar to the uterus lining (endometrium) grows outside the uterus. It usually grows in your pelvis but can occur in almost any part of the body.
The hormone oestrogen can cause this tissue to grow and break down when you have your period. This can lead to pain and inflammation. There can also be scarring, causing organs to stick together (known as adhesions).
Endometriosis is a progressive and chronic condition, meaning it gets worse over time. It can be very painful and can affect fertility. In Australia, around 1 in 9 females develops endometriosis and can experience symptoms even after menopause.
There is no cure for endometriosis but there are treatments to relieve symptoms.
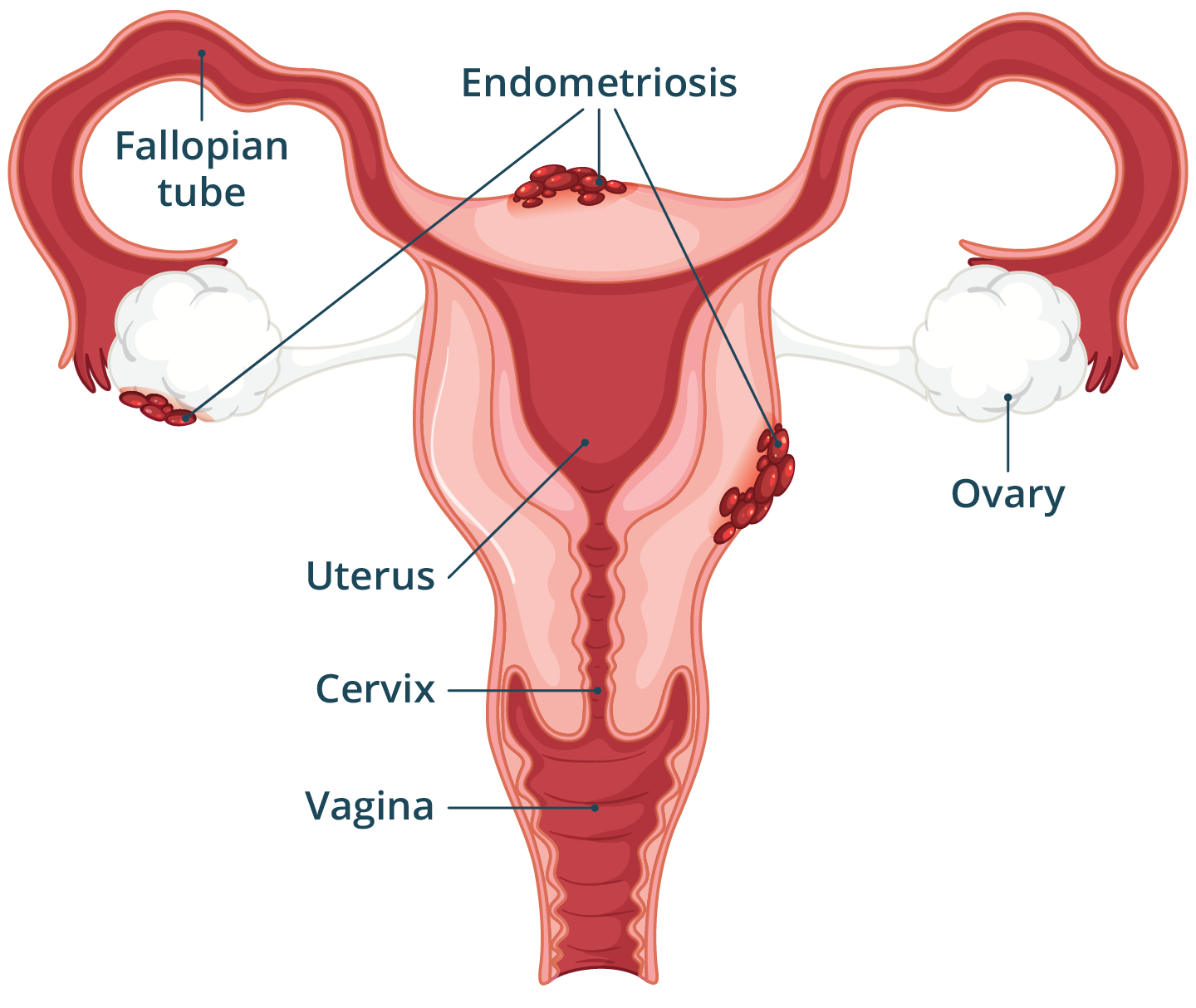
What are the symptoms of endometriosis?
People with endometriosis will experience different symptoms. Depending on where the endometriosis is, the severity of symptoms will vary.
Symptoms include:
- abdominal (tummy) or pelvic pain with your period, sex or going to the toilet
- pain in your thigh or leg, which may get worse over time
- heavy periods or irregular bleeding
- bleeding from the bladder or bowel, or changes in urination (weeing) or bowel movements (pooing)
- feeling bloated, with or without pain
- being tired, especially around the time of your period
- not being able to get pregnant (infertility)
For some people, the pain is so severe that they cannot take part in education, work or sport. Sometimes, the pain of endometriosis is associated with anxiety or depression.
For advice and to get connected to local mental health services, call Medicare Mental Health on 1800 595 212. Check the operating times
What causes endometriosis?
Doctors don't know what causes endometriosis. There are some things that put you at greater risk:
- Retrograde menstruation. This is when menstrual (period) blood travels backwards into the pelvis. Cells in the blood can stick onto pelvic organs and grow.
- Your immune system. A weak immune system may mean that your body cells can't properly remove menstrual tissue that flows backward into the pelvis.
- Family history. People who have a close relative with endometriosis are more likely to also develop it.
Other possible contributing factors for endometriosis include:
- long and heavy periods
- frequent periods or short cycles
- starting your period before 11 years of age
- having your first pregnancy when you are older
- low body weight
When should I see my doctor?
If you think you have endometriosis, talk to your doctor about your symptoms. Even with treatment, your pain and endometriosis may come back. Ask your doctor about the pros and cons of all your treatment options.
ASK YOUR DOCTOR — Preparing for an appointment? Use the Question Builder for general tips on what to ask your GP or specialist.
The Raising Awareness Tool for Endometriosis (RATE) can help you and your doctor look for symptoms of endometriosis. This may help you get a diagnosis faster and start treatment sooner.
How is endometriosis diagnosed?
Many people learn they have endometriosis when they see a doctor for fertility problems or have surgery for other reasons. For some, this means a delay of several years between first having the condition and getting a diagnosis.
To diagnose endometriosis, your doctor will ask about your symptoms and examine you. They may recommend an ultrasound, MRI scan or laparoscopy. A laparoscopy is a type of surgery where a small scope (camera) looks through small cuts made in your abdominal (tummy) wall. This lets your doctor see inside your pelvis and collect some tissue to test for endometriosis.
There are 4 stages of endometriosis: minimal, mild, moderate and severe. The stage depends on the location and amount of endometriosis you have. A higher stage doesn't always mean you will have more pain.
How is endometriosis treated?
If you have endometriosis, you may have a team of healthcare professionals available to help you. There are endometriosis and pelvic pain clinics around Australia to help with treatment options and services.
To treat endometriosis, you might have medicine, surgery or other treatments.
Medicines for endometriosis
Treatment will depend on:
- your symptoms
- how severe your endometriosis is
- whether you want to become pregnant
Medicines for endometriosis include hormone-based treatments such as:
- oral contraceptive pill ('the pill')
- contraceptive implant
- intrauterine device (IUD)
- progestogen pill (such as dienogest)
- gonadotrophin-releasing hormone analogues (GnRHa)
- relugolix combination therapy (such as ryeqo)
Some of these medicines are on the Pharmaceutical Benefits Scheme (PBS). This can help you access the medicine at a lower cost. Speak to your doctor about your options and which medicine is best for you.
Hormone treatments can reduce symptoms and limit the growth of endometrial cells. Because they work only as long as you take them, the endometriosis may come back if you stop taking the medicine.
Hormone therapy is not suitable in some situations. Tell your doctor if you are planning a pregnancy before starting treatment.
Your doctor may also recommend that you take pain-relief medicines.
Surgery for endometriosis
Surgical treatment aims to remove as much of the endometriosis as possible.
One option is laparoscopic (keyhole) surgery. The doctor makes a small cut in your abdomen to remove the endometrial tissue.
Sometimes, your doctor may recommend removing your uterus (a hysterectomy), but this doesn't always stop the pain.
Other treatment options
Sometimes your doctor may recommend a combination of medicine and surgery. You can also try other treatments like physiotherapy or psychology.
Always check with your doctor or pharmacist before you use complementary treatments, as they may interfere with prescribed medicines.
To help with your endometriosis, try to get enough sleep, stay active, and find ways to reduce stress.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
What are the complications of endometriosis?
Endometriosis can cause bladder and bowel issues. Pelvic floor exercises can help ease these symptoms, as well as chronic pain.
Ask your doctor to refer you for pelvic floor physiotherapy, or to a psychologist or pain clinic to help you find the right strategies to manage chronic pain.
Around 1 in 3 females with endometriosis have trouble with fertility. Fertility treatment, such as in vitro fertilisation (IVF) can often help. Ask your doctor for a referral if you have endometriosis and are having trouble becoming pregnant.
Surgical complications of endometriosis treatment include recurrence of painful periods, pain during sex and rectovaginal fistula (abnormal connection between the rectum and vagina).
Resources and Support
Visit the Jean Hailes for Women's Health website for more information.
Endometriosis Australia has information, including fact sheets, a podcast and a range of support groups you can connect to.
Endozone has research-based information and tips on managing endometriosis symptoms through different life stages — from school to work and family life. It also has useful resources for people living with endometriosis and those who support them.
Do you prefer to read in languages other than English?
Jean Hailes for Women's Health has factsheets available in a range of community languages.
Looking for information for Aboriginal and/or Torres Strait Islander people?
Find an Aboriginal Community Controlled Health Organisation (ACCHO) or Affiliate near you.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: July 2025





















