Plantar fasciitis
Key facts
- Plantar fasciitis is when the tissue on the bottom of your foot (the plantar fascia) becomes inflamed.
- This can cause heel pain and discomfort when walking.
- You may be at risk of plantar fasciitis if you do physical activity that places stress on your heel.
- If you think you have plantar fasciitis, see your doctor.
- Your doctor can suggest treatments, such as stretches, pain medicines and supportive shoes.
What is plantar fasciitis?
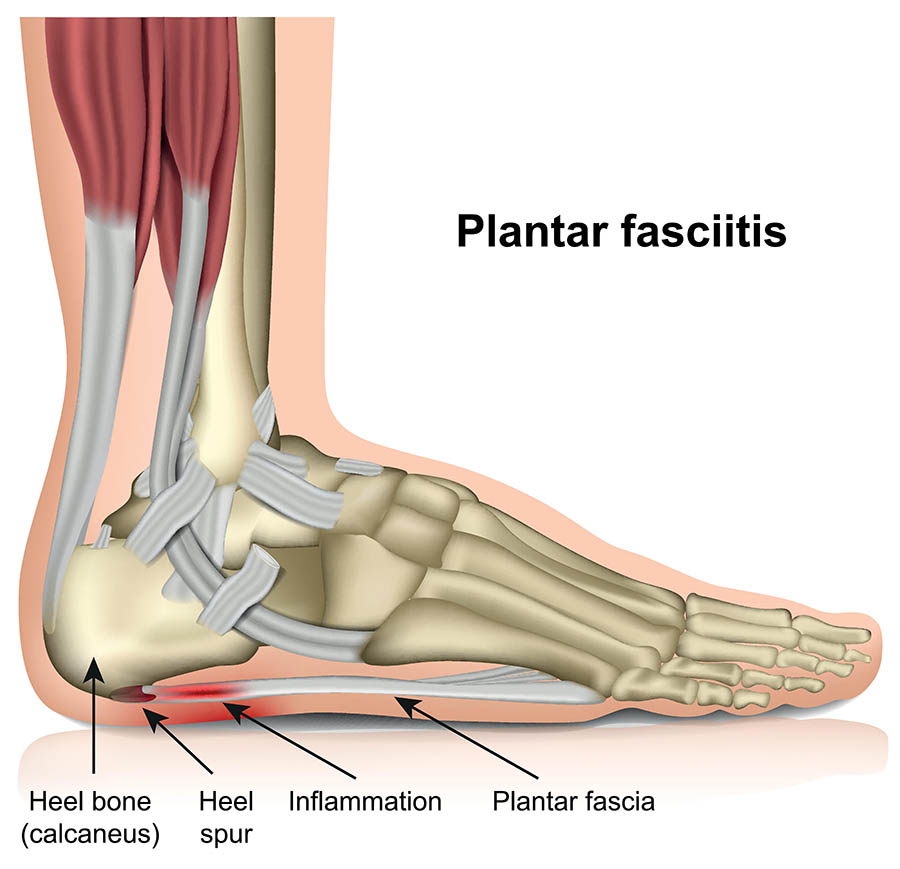
The plantar fascia is a piece of strong, thick tissue that runs along the bottom of your foot. It connects your heel bone to your toes. This helps to create the arch of the foot and keeps the bones in place.
Plantar fasciitis happens when your plantar fascia becomes sore.
Plantar fasciitis is often associated with a heel spur. This is a spike of bone poking out from the heel bone. Many people have heel spurs without any pain.
What are the symptoms of plantar fasciitis?
The main symptom of plantar fasciitis is pain under your heel. This pain can be dull or sharp. You may also notice:
- aching or burning on the sole (bottom) of your foot
- swelling in your heel
The pain is often worse:
- in the morning, as you take your first steps
- after long periods of standing or sitting
- after doing a lot of activity
CHECK YOUR SYMPTOMS — Use the Symptom Checker and find out if you need to seek medical help.
What causes plantar fasciitis?
Plantar fasciitis can be caused by sports and activities that put stress on your heel bone. This can include:
- running
- dancing
- aerobics
- other activities that involve jumping
Plantar fasciitis is more likely to happen if you increase the amount of these activities or start a new form of exercise.
It can also be caused by:
- being flat-footed
- having high arches
- being middle-aged or older
- being overweight or pregnant
- spending a lot of time on your feet
- wearing shoes with poor arch support or changing in footwear
- having tight or weak calf muscles
When should I see my doctor?
If you have symptoms of plantar fasciitis that last for longer than 8 weeks, see your doctor. They can diagnose your condition and advise you on the best treatment. If needed, they can refer you to a specialist.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How is plantar fasciitis diagnosed?
If your doctor thinks you might have plantar fasciitis, they will ask you some questions about:
- your symptoms
- the type of work you do
- your lifestyle — the amount and type of physical activity that you do
They will probably look at your feet and your calves. They will check to see if there is any:
- discomfort
- tightness
- weakness
They may also refer you for an x-ray or ultrasound scan to rule out other causes of heel pain. However, this is often not needed for diagnosis.
How is plantar fasciitis treated?
Plantar fasciitis can often last for weeks or months.
Self-care at home
To help treat pain caused by plantar fasciitis, you can:
- rest your foot as much as possible
- apply an icepack to your foot for 10 to 20 minutes up to 4 times a day
- wear shoes with good support and cushioning
- insert heel pads or arch supports (orthotics) in your shoes
- apply supportive taping before activity
- shockwave therapy, which can be performed by a specialist to help with healing
They may also suggest some exercises for you to do to stretch your plantar fascia. This can help you to better absorb your body weight.
Medicines for plantar fasciitis
Your doctor may suggest that you take pain-relief medicine, such as ibuprofen or paracetamol
Other treatment options
If these measures don't work, your doctor may:
- give you steroid injections in your heel
- suggest surgery
These treatments are rare and usually only used in the most severe cases.
Can plantar fasciitis be prevented?
There are ways to reduce your risk of plantar fasciitis. Try to:
- maintain a healthy weight
- choose supportive shoes
- warm up before any activity
- rest between physical activities
- avoid activities that cause pain
- introduce exercise, such as running, gradually
What are the complications of plantar fasciitis?
Plantar fasciitis can make it painful to walk. If you are walking differently to help with the pain, this may cause other complications and slow your recovery. If your heel pain is affecting your day-to-day activities, see your doctor.
Resources and support
If you need to know more about plantar fasciitis, you can:
- Visit the Sport Medicine Australia website to learn more about plantar fasciitis.
- Call the Musculoskeletal Health Australia helpline on 1800 263 265.
You can also call the healthdirect helpline on 1800 022 222 (known as NURSE-ON-CALL in Victoria). A registered nurse is available to speak with you 24 hours a day, 7 days a week.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: March 2025













