Electrocardiogram (ECG)
Key facts
- An electrocardiogram is a simple, painless test that measures your heart's electrical activity.
- An electrocardiogram is also known as an ECG or EKG.
- Your doctor may advise that you have an ECG test if you have chest pain or a racing heart.
- If your ECG is abnormal, you may need further tests or treatment.
What is an ECG?
An electrocardiogram is a graph of your heart's electrical activity. It's also known as an ECG or EKG. An ECG test is simple, safe and painless.
The ECG graph can help your doctor make a diagnosis. There's no risk of being electrocuted.
What are the benefits of an ECG?
Your doctor may recommend an ECG test if you have chest pain, a racing heart or other heart problems.
An ECG can show if you are having or have had:
- a heart attack
- a stressed heart muscle, due to narrowing or blockages in your heart arteries
- irregular heart rhythms
- pericarditis (heart lining inflammation)
- abnormal heart electrical pathways
An ECG tells your doctor if your heart medicines are working properly.
ASK YOUR DOCTOR — Preparing for an appointment? Use the Question Builder for general tips on what to ask your GP or specialist.
What does an ECG test involve?
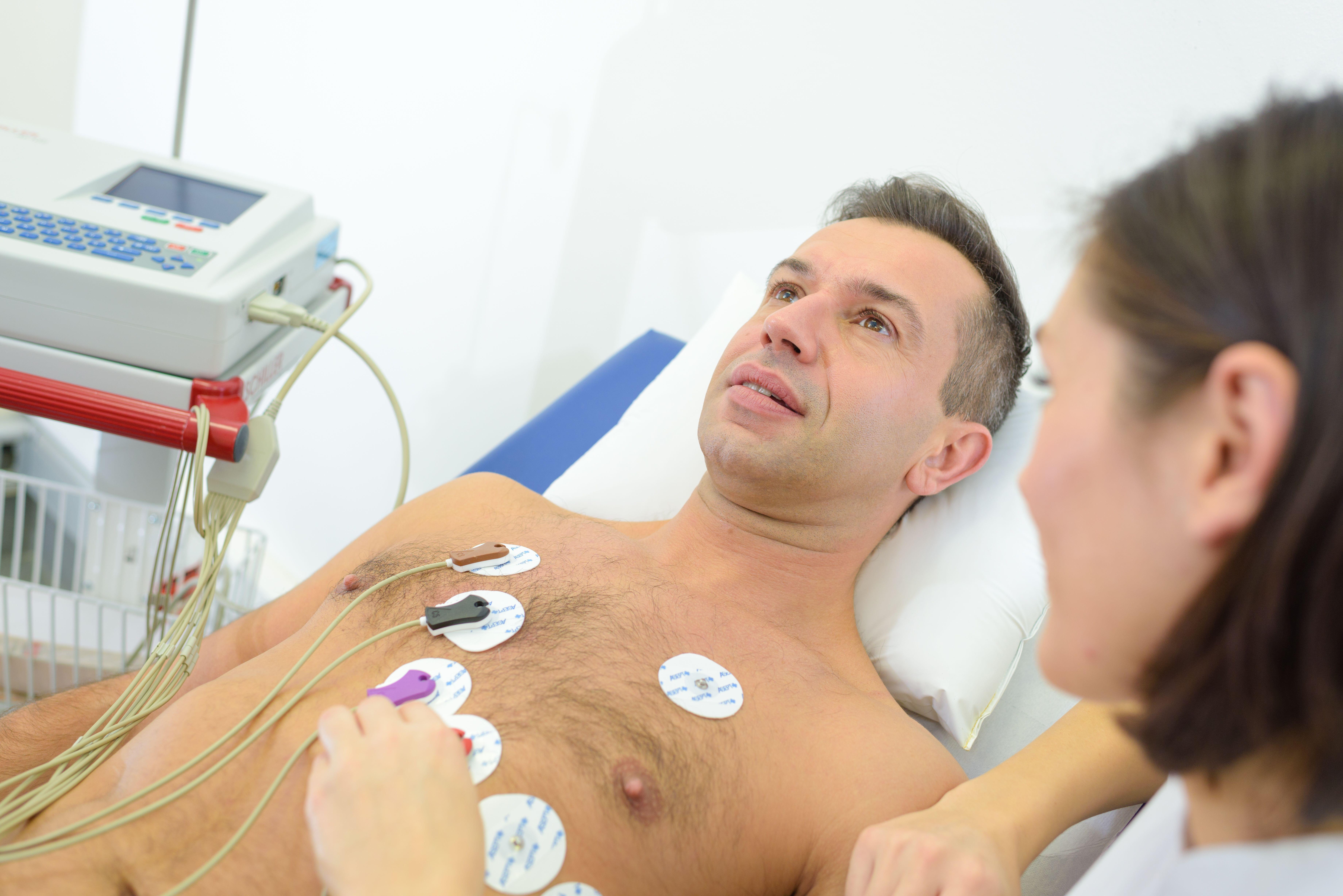
During an ECG test, 10 leads are attached to electrodes using sticky dots. These are placed on your:
- arms
- legs
- chest
The leads connect to a machine, which takes the reading.
What are the different types of ECG test?
There are a number of different types of ECG test.
- Resting ECG: you lie still and relax for a few minutes while the ECG is recorded. You should breathe normally.
- Ambulatory ECG (also called a 24-hour ECG, or Holter monitor): you wear the leads and carry a monitor while you go about your usual activities for at least 24 hours.
- A cardiac stress test: the ECG is recorded while you exercise on a treadmill. It checks for areas of heart muscle that struggle when stressed. If you cannot exercise, medicines might be used to test the effect of stress on your heart.
If you have chest pain or another problem during the ECG, it's important to tell the technician doing the test.
If you're having an ambulatory ECG, the technician may give you a diary to record any symptoms.
Who will perform my ECG?
Your ECG could be done by a:
- nurse
- ECG technician
- doctor
A trained doctor or nurse will look at the ECG pattern and interpret what it says about your heart.
What happens after an ECG test?
Your doctor will discuss the results with you.
If your doctor notices a serious problem in your ECG, you may need to begin treatment.
Sometimes you may need other tests, like:
- an ultrasound of your heart (echocardiogram)
- blood tests
- an angiogram (pictures of the heart's blood vessels)
How can I prepare myself for an ECG test?
You don't need to do anything special before your ECG appointment. The test will take about 30 minutes.
Think about any questions you might have for the doctor or ECG technician doing the test.
Before your ECG, the technician will make sure that the electrodes will stick on your body. They may shave or clean areas of your chest, arms or legs.
You might be asked to take off your bra or any metal jewellery.
How soon will I recover?
No recovery time is needed after a resting or ambulatory ECG test.
The technician or doctor will remove the leads and equipment. You may need to rub off any adhesive (glue) left on your skin.
Depending on your fitness level, you will need a few minutes rest after the cardiac stress test. This is for your heart rate to return to normal after exercising.
What complications can happen?
There are no major complications from an ECG. It's a safe and painless test. You could have a minor skin reaction to the adhesive gel, but it should get better quickly.
During the cardiac stress test, you may get out of breath or experience chest pain. If this happens, tell the technician or doctor straight away.
Are there alternatives to an ECG?
Your doctor can check your pulse (heart rate), listen to your heart with a stethoscope and take your blood pressure without doing an ECG. These things give them some information about your heart.
An ECG gives your doctor much more detail about how well your heart is working. An ECG test is a very useful source of information for your doctor.
The Holter monitor (ambulatory ECG) provides round the clock monitoring. The resting ECG gives you information about what your heart is doing during the test.
Should I use a smartphone or smartwatch ECG application?
Some heart problems are hard to diagnose if your symptoms don't happen while you're having the ECG.
Some smartphone and smartwatch applications (apps) can generate an ECG. If you often wear a smartwatch this could be useful. You can mention this to your doctor, who may find the tracking information useful.
However, apps are less accurate than an ECG test.
What will happen if I decide not to have the ECG test or it is delayed?
Your doctor will continue to monitor your symptoms. They may assess your risk factors for heart problems.
If you refuse an ECG it could take longer to find out if you have a serious problem such as a heart attack or heart rhythm problem. In an emergency it could even mean the difference between life and death. If you can get a fast and accurate diagnosis of a heart condition from an ECG, treatment can be started more quickly.
Resources and Support
Visit the Heart Foundation website for information and resources about heart health.
You can also call the healthdirect helpline on 1800 022 222 (known as NURSE-ON-CALL in Victoria). A registered nurse is available to speak with 24 hours a day, 7 days a week.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: May 2025













