Chilblains (perniosis)
What are chilblains?
Chilblains are itchy, swollen and painful lumps or patches on your skin. They form after exposure to cold but not freezing temperatures. They usually affect the fingers, and toes but can also appear on the nose and ears.
Chilblains are sometimes called 'perniosis'.
Chilblains do not cause lasting damage. They usually heal in a few weeks. They're not the same as frostbite, which is more serious. The affected area might stay sensitive to cold after they heal.
What are the symptoms of chilblains?
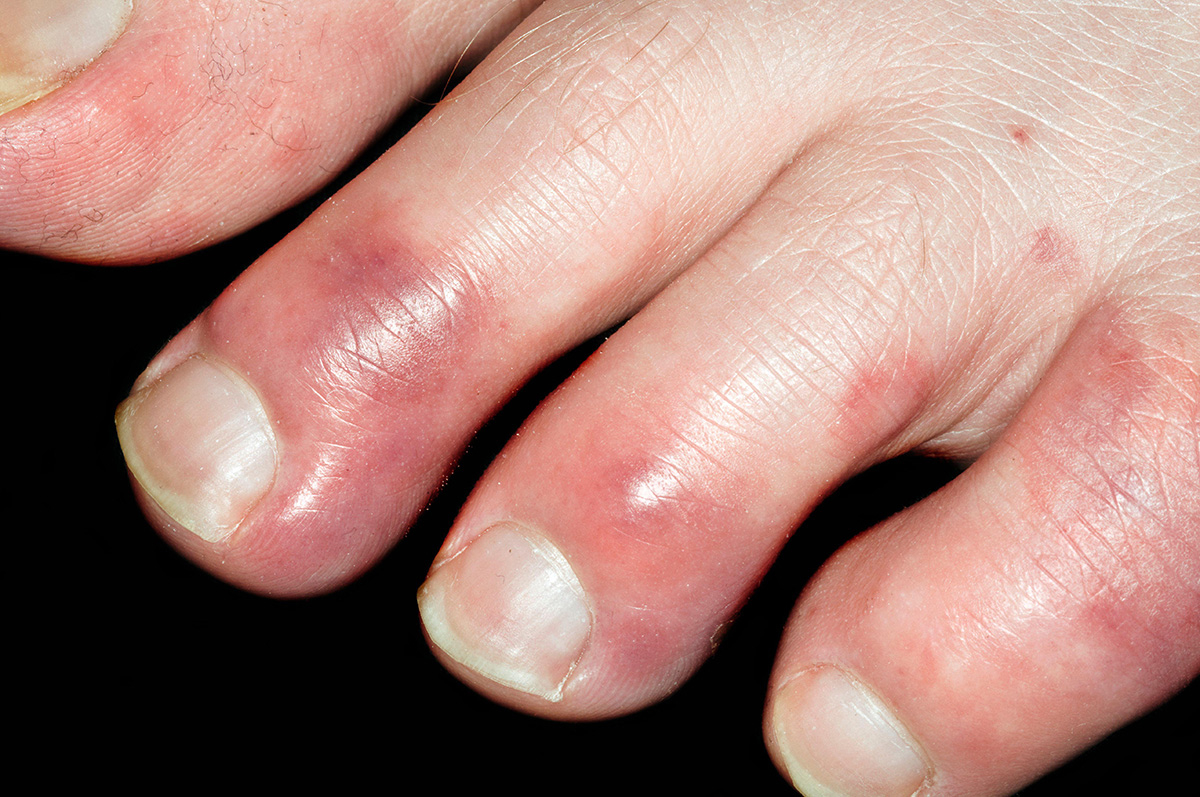
Chilblains appear as reddish-purple bumps or patches on the skin.
Chilblains can appear quickly, most often on your fingers or toes. Other areas that can be affected include your heels, sides of the feet, nose, ears or thighs.
Other symptoms of chilblains include:
- itching or burning
- swelling
- pain
Blisters containing clear fluid may also form.
Chilblains normally disappear in 1 to 3 weeks.
CHECK YOUR SYMPTOMS — Use the Symptom Checker and find out if you need to seek medical help.
What causes chilblains?
Chilblains are areas of inflammation and swelling of your skin.
Chilblains are caused by changes to your blood vessels in response to the cold. You are more likely to develop chilblains if you are sensitive to the cold.
They can also form due to poor circulation or sensitive skin.
Other risk factors for getting chilblains include:
- exposure to damp and wind
- having a low body weight
- being female
- being a child, teenager or older person
When should I see my doctor?
See your doctor if your symptoms are ongoing or you can't get your pain under control. Also see your doctor if you have a lot of chilblains.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How are chilblains diagnosed?
Your doctor will ask about your symptoms and examine the affected skin.
Your doctor can usually diagnose chilblains if you tell them you have been exposed to damp, cold conditions.
Occasionally, a blood test or sample of the lesion may be recommended. This is to rule out other conditions.
How are chilblains treated?
The best treatment is staying warm and protecting your affected skin. You need to keep your whole body warm, not just your feet and hands. This keeps your warm blood circulating.
Other self-care measures include the following:
- Try to avoid scratching, which can cause infection.
- Use a moisturiser to relieve the itching.
- Massage the affected area if it's not too painful or ulcerated.
Once you have had chilblains they can come back. This can happen even after brief exposure to cold. So, it's important to stay warm.
Your doctor might suggest or prescribe:
- corticosteroid cream or ointment to reduce itching and swelling
- applying dressings to the affected skin
- medication or patches to expand the blood vessels and increase blood flow to the affected areas
Can chilblains be prevented?
You can lower your risk of getting chilblains by:
- keeping your hands, feet and body warm
- avoiding cold, damp and windy conditions
- exercising regularly to improve your circulation
- not smoking, as this affects your circulation
Wear loose, warm clothes that cover your arms and legs. Wear gloves on your hands to help prevent chilblains on your fingers. And thick socks with closed shoes to help prevent chilblains on your toes.
If you have severe chilblains that keep coming back, you may be advised to take medicine when the weather is cold. This will help to prevent chilblains returning. Talk to your doctor about whether this may be suitable for you.
What are the complications of chilblains?
Very rarely, chilblains may be associated with blood or bone marrow disorders, or diseases like lupus or Raynaud's disease.
Chilblains may also be a sign you have peripheral vascular disease, which reduces blood flow to the feet and hands.
Resources and support
More information about circulation is available on Blood and blood vessels article.
If you need to know more about chilblains, or to get advice on what to do next, call healthdirect on 1800 022 222 to speak with a registered nurse, 24 hours, 7 days a week.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: June 2022













